How to Get Good Care Wherever You Go
Last updated July 2016
 Regardless of which hospital you are admitted to, you and your family or friends can do a lot to influence the quality of care you receive. What matters most is your attitude. It is important that you feel involved in, and responsible for, your own care—that you view the hospital and staff only as the setting and the means to help you get well.
Regardless of which hospital you are admitted to, you and your family or friends can do a lot to influence the quality of care you receive. What matters most is your attitude. It is important that you feel involved in, and responsible for, your own care—that you view the hospital and staff only as the setting and the means to help you get well.
Before You Arrive
If there is time, a little care in getting ready for your hospital stay will serve you well later on.
If you will be getting care from a surgeon or other specialist, meet with this doctor. Get a full explanation of exactly what will be done. Get an understanding of who will be doing your surgery and what role assistants might play. Find out who will be caring for you as you recover after surgery and after you leave the hospital. If you are not happy with the answers, this would be the time to change doctors.
If you will be having surgery, try to meet also with the anesthesiologist. It is better to have this meeting in the more relaxed atmosphere of an office visit than to meet with the anesthesiologist, in the typical way, for a few hurried minutes right before the operation. Arranging an appointment in advance is not easy to do (and be sure to confirm that your insurance will cover it), but it is worthwhile, given the importance to your safety of his or her work. You can ask your surgeon to give you the name of the anesthesiologist and to help you make an appointment. When the anesthesiologist asks questions, be sure to give thorough answers—about high blood pressure, heart problems, allergies, or other conditions that might put you at risk when under anesthesia. Also, confirm that the anesthesiologist, not a subordinate, will actually be present with you in the operating room.
 If you might need blood transfusions in connection with surgery, ask your surgeon whether autologous transfusion makes sense for you—giving your own blood and having it stored for your own later use. You might be able to give a unit a week for several weeks before surgery.
If you might need blood transfusions in connection with surgery, ask your surgeon whether autologous transfusion makes sense for you—giving your own blood and having it stored for your own later use. You might be able to give a unit a week for several weeks before surgery.
Decide whether you will want a private or semi-private room. With a private room, you avoid any problems with roommates who might be noisy or have annoying visitors. But sharing a room with someone else gives you a little company, is likely to increase the frequency of nurse visits to your room since there are two patients to visit, and gives you someone who might be able to call for help for you in a crisis.
Think carefully about packing for the hospital. Be sure to take a toilet kit with toothbrush, shampoo, deodorant, and other items just as you would if you were going on a vacation. Bring pajamas, a robe, and non-skid slippers.
Don’t bring valuables. You will not be able to keep an eye on them all the time—certainly not when you are in surgery or recovery. Don’t bring more than a few dollars in cash, but do bring a credit card and your phone. You might want to bring a few pictures to keep you company and possibly a few other items of sentimental value, but don’t bring keepsakes you don’t want to lose.
Check in advance with your doctor which of your regular medications, including vitamin supplements, you will be continuing to take while in the hospital. Bring a list of these medications, noting the dosage and frequency. If you bring the actual medications, have your doctor mark in your medical record that you are to take these medications and that the nurses are to find a place to store them; be sure to label them clearly as yours. Bring them in their original bottles with labels.
Make arrangements for where you will go and how you will be cared for after discharge. You may not know in advance what condition you will be in after release, but it is wise to talk with your doctor about the possibilities and to make at least preliminary arrangements.
Monitor Your Own Care
 Learn as much about your condition as possible before going to the hospital by talking to your doctor and doing research in libraries and on the Web. Ask your doctor to tell you what treatment is recommended, what alternatives are available, and the consequences of each. Find out what medications, if any, you will be taking, what they look like, and any possible side effects. If you and your doctor go over these things before you are in the hospital, you will be better prepared to deal with each treatment step and less likely to be surprised or feel pressured about making decisions.
Learn as much about your condition as possible before going to the hospital by talking to your doctor and doing research in libraries and on the Web. Ask your doctor to tell you what treatment is recommended, what alternatives are available, and the consequences of each. Find out what medications, if any, you will be taking, what they look like, and any possible side effects. If you and your doctor go over these things before you are in the hospital, you will be better prepared to deal with each treatment step and less likely to be surprised or feel pressured about making decisions.
During treatment, keep notes on the results of tests. Also keep track of changes in medications or diet and their effects.
Write down questions you want to ask the doctor or the unit’s head nurse during his or her visit and record the answers.
By keeping track of these things, you will know more about your condition and what to expect. You will also know enough to question the arrival of an unexpected meal or a new pill. It may not be yours.
Be Yourself
 Simply as a part of being in the hospital, many people become more passive and dependent than usual. Inactivity and concern about your condition contribute to this; so does the typical hospital routine of frequent interruptions and continual waiting—for meals, tests, visits from the doctor and friends, and medication. To help you be yourself, try to personalize your day and your surroundings by putting out a few personal (not valuable) items from home, by wearing your own clothes where possible, by calling friends and asking them to bring you snacks (provided you are not on a restricted diet), or by doing some work or reading. If not disruptive to others or harmful to your condition, these kinds of activities might help you resist becoming excessively reliant on the hospital and staff—and will help to ensure that staff members regard you as a person, not just a case. We know one patient who purposely wore bright red pajamas and did aerobic exercises every day just so she would not be typed simply as “thyroid tumor in 302.”
Simply as a part of being in the hospital, many people become more passive and dependent than usual. Inactivity and concern about your condition contribute to this; so does the typical hospital routine of frequent interruptions and continual waiting—for meals, tests, visits from the doctor and friends, and medication. To help you be yourself, try to personalize your day and your surroundings by putting out a few personal (not valuable) items from home, by wearing your own clothes where possible, by calling friends and asking them to bring you snacks (provided you are not on a restricted diet), or by doing some work or reading. If not disruptive to others or harmful to your condition, these kinds of activities might help you resist becoming excessively reliant on the hospital and staff—and will help to ensure that staff members regard you as a person, not just a case. We know one patient who purposely wore bright red pajamas and did aerobic exercises every day just so she would not be typed simply as “thyroid tumor in 302.”
In general, do all you can for yourself. No one expects you to jump out of bed hours after you come out of the operating room. But as you and your doctor feel you are able, try to feed yourself, get out of bed by yourself, and generally take on as much as you can of your own care. This is therapeutic for you and will gain you the respect of the staff.
Be sure to express your appreciation for the good care you receive. Nurses have a demanding job and, like everyone else, need a little feedback. If one of your visitors can bring a gift or some flowers for the nurses, rather than for you, that will be appreciated. Also, learn your nurses’ names and call them by name.
Protect Yourself
Given the high risks of infections, drug errors, and other hospital mishaps, it is essential that you take steps to protect yourself. If this means you are not the most agreeable patient, so be it. This is a matter of life and death.
Protect Yourself from Infections
 Hospital-caused infections are a major killer—and a major cause of suffering, anxiety, and extended hospital stays. Most infections are the result of the spreading of “germs” from patient to patient on the hands of physicians, nurses, and other hospital workers. The best way to reduce this problem is very low-tech: the people who touch you in the hospital just need to wash their hands. Numerous studies have demonstrated that handwashing sharply reduces rates of patient infections. Although this has been known for 150 years, hospital workers simply don’t always follow the basic rules of hygiene. Most healthcare workers understand the importance of handwashing but simply don’t do it consistently—and aren’t even aware of how poorly they are doing.
Hospital-caused infections are a major killer—and a major cause of suffering, anxiety, and extended hospital stays. Most infections are the result of the spreading of “germs” from patient to patient on the hands of physicians, nurses, and other hospital workers. The best way to reduce this problem is very low-tech: the people who touch you in the hospital just need to wash their hands. Numerous studies have demonstrated that handwashing sharply reduces rates of patient infections. Although this has been known for 150 years, hospital workers simply don’t always follow the basic rules of hygiene. Most healthcare workers understand the importance of handwashing but simply don’t do it consistently—and aren’t even aware of how poorly they are doing.
The solution for you? Ask every healthcare worker—including doctors—to wash his or her hands before touching you, your food, your medications, or equipment that will come into contact with you. Studies have found that one of the most effective ways—better than training programs or rewards and punishments—to get healthcare workers to wash their hands is for patients to ask them to do so.
Washing hands with disinfectant soap and water is one effective technique. But it takes 15 to 30 seconds to do it right; it takes time for the hands to dry; and washing hands many times per day can be irritating to the skin. A faster, less irritating, and equally effective alternative is hygienic handwipes.
Take to the hospital with you a supply of sanitizing handwipes, which you can buy in the drug store, and keep them in a prominent place at your bedside. These alcohol-based handwipes generally have emollients that make them easy on the skin.
 You may feel awkward interfering in the healthcare workers’ routines. Overcome it. Be polite, but not passive. The stakes are too high. Some hospitals have found that instructing patients at admission to ask every healthcare worker to wash his or her hands is an effective way to increase handwashing compliance. But hospitals don’t typically take this approach. You need to do it on your own. You can simply explain that you are doing as you were told by an article you read.
You may feel awkward interfering in the healthcare workers’ routines. Overcome it. Be polite, but not passive. The stakes are too high. Some hospitals have found that instructing patients at admission to ask every healthcare worker to wash his or her hands is an effective way to increase handwashing compliance. But hospitals don’t typically take this approach. You need to do it on your own. You can simply explain that you are doing as you were told by an article you read.
Ask also about equipment that will come into contact with you. That stethoscope should also be cleaned with a sanitizing wipe. Contaminated catheters, infusion pumps, endoscopes, and bronchoscopes can also be a problem, though one you will have a harder time monitoring.
If your roommate or the roommate’s visitors show signs of contagious illness, like sneezing or coughing, ask your doctor about changing rooms.
Protect Yourself Against Drug Errors
The Institute of Medicine report, To Err Is Human, highlighted the shocking frequency of medication errors in hospitals. The institute cited numerous studies to document the problem. For example, one study of a 37-day period in a sophisticated urban hospital found 27 cases of “injury resulting from a medical intervention related to a drug.”
Hospitals could do, and long since should have done, much to reduce this problem, including the introduction of Computerized Physician Order Entry (CPOE) systems. But there is also a lot you can do to protect yourself.
The key is to have a written list of the medications—including medications taken via IV hookup—you will be receiving, why, how often, and what the proper dosage is. If a medication looks different from what you have been getting, stop and ask the nurse about it. Maybe it is just a generic-equivalent substitute, but maybe it is the wrong drug. Be sure the hospital staff knows about all the medications you and your doctors have agreed you will be taking.
Make notes of when you get medications. If you don’t get one on schedule, ask the nurse why not. You and the nurse can confirm the missed dose by checking your chart.
If you have an unexpected reaction to a drug, bring it to the attention of the nurse immediately. Some, but not all, of the types of reactions to look out for are tightness in your chest, shortness of breath or trouble breathing, pain, burning sensations, dizziness, confusion, numbness, or itching.
Avoid Falling
 Hospital patients are at substantial risk of falling, even patients who are young and strong and would not normally be considered to be at risk. You may be weak from illness or injury or from too much time in bed, or you may be dizzy or confused from medications. Falls can cause hip fractures, other types of fractures, concussions, or other injuries.
Hospital patients are at substantial risk of falling, even patients who are young and strong and would not normally be considered to be at risk. You may be weak from illness or injury or from too much time in bed, or you may be dizzy or confused from medications. Falls can cause hip fractures, other types of fractures, concussions, or other injuries.
There are various precautions you can take to avoid falling—
- Before getting out of bed, sit still on the edge of the bed with your feet dangling until you are sure you have your balance. If you still feel at all unsteady, call a nurse or aide to help—and wait for the help.
- If you have been instructed not to get up without help, follow that instruction.
- Keep your eyeglasses by the side of your bed. Be sure you can see normally, that your vision is not suffering from side effects of treatment, before trying to walk.
- Wear slippers that have non-skid soles and that will stay on your feet. If there are wet spots on floors, ask someone to dry them before proceeding.
- Make sure that furniture is not in your way. Before going to bed at night, check that furniture is arranged so that it won’t interfere with you if you have to go to the bathroom.
- Take your time. Even a few days in the hospital can sap your strength. Use a walker if that will help.
- Don’t get out of bed until your bed is cranked down and never try to climb over raised side rails. Ask a nurse or aide to fix your bed so that you can get out.
Be Able to Get Help When You Need It
 When you first arrive in your room, locate the call buttons at bedside and in the bathroom. Tell the nurses that you want to test them, and do so.
When you first arrive in your room, locate the call buttons at bedside and in the bathroom. Tell the nurses that you want to test them, and do so.
When you use a call button, you should expect an immediate response—at least by intercom—to find out how urgent your need is.
If you don’t get a quick enough response, call again. If you feel desperate, use your outside phone line to call the hospital and ask to be connected to the nursing station that serves your room number. If that, too, fails to get a response, call your doctor.
Insist on Attentive Nursing Care
Expect at least the following from the nursing staff—
- Nurses should observe you every few hours if you are not seriously ill—every few minutes if you are critically ill.
- They should spend time with you to ask about any changes in your condition, any pain, any new complaints.
- They should call your doctor if an unexpected change occurs—or if you are concerned enough that you think the doctor should know.
- There should be some continuity of the nursing staff—not a constant daily turnover of new faces.
Don’t Get Cut in the Wrong Place
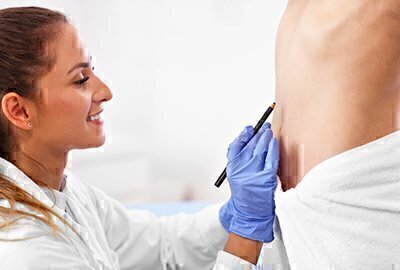 Wrong-site surgery—operating on the wrong body part—is the kind of mishap that gets dramatic attention in the press. Fortunately, it is not very common. Unfortunately, it is still too common.
Wrong-site surgery—operating on the wrong body part—is the kind of mishap that gets dramatic attention in the press. Fortunately, it is not very common. Unfortunately, it is still too common.
A key measure to avoid such catastrophes is to mark the surgery site with a permanent marker, during a preoperative visit, before the day of the operation. Such marking has become standard procedure among competent health care providers. For example, in 1998, the American Academy of Orthopaedic Surgeons endorsed a surgical site identification program called “Sign Your Site.” Ask your surgeon what site-marking procedure he or she uses, and then mark the site together while you are at the doctor’s office.
Take Charge of Communication
Be sure the nursing staff knows about your conditions—what you are in the hospital for and other conditions that might affect the care you should receive. Hospitals are big places. Hospital workers care for dozens of patients every day. One worker takes over when another worker goes home. A lot of information can get lost in the shuffle; confusion can ensue. Computerized medical records, if properly used, would help. But many hospitals are still shamefully backward in implementation of such systems, relying instead on the same types of patient records they have used for many years. It is, unfortunately, important for you, if you are able, to keep track of what is going on and make sure the right information gets from one caregiver to another.
First, make sure they know who you are. Make sure your wristband is accurate. To help everyone keep things straight, use a piece of posterboard to make a sign with your name, serious allergies, and chronic medical conditions and post it at the head of your bed. Some hospitals actually supply posters for this purpose.
Be particularly vigilant at shift changes—to be sure the new folks know what went on, or didn’t go on, during the previous shift. The sign-out procedures used in most hospitals when a physician goes off duty to pass information to the “cross-covering” physician who will take care of patients in the interim are often informal and unstructured. Errors are more likely to occur during the coverage period of the cross-covering physician than when the regular physician is on duty.
Keep a log of what happens to you each day. If something seems to have been missed, or if there is an attempt to repeat some test or treatment that you think is unnecessary because it has already been done, ask about it. Refer to your log and your medical record.
Eat Right
 Eating right is important for you to feel right when you are at home, so it’s not surprising that it is also important when you are in a hospital. Unfortunately, that is not always easy. The food often leaves a lot to be desired. If the food is not as hot or as cold as it should be, ask the staff if that can be improved. If you find it just too unpleasant to eat, ask your doctor to authorize you to get food from the outside and ask friends to bring meals to you. Ask to have a small space arranged for you to store your food in a hospital refrigerator. Be sure to label it.
Eating right is important for you to feel right when you are at home, so it’s not surprising that it is also important when you are in a hospital. Unfortunately, that is not always easy. The food often leaves a lot to be desired. If the food is not as hot or as cold as it should be, ask the staff if that can be improved. If you find it just too unpleasant to eat, ask your doctor to authorize you to get food from the outside and ask friends to bring meals to you. Ask to have a small space arranged for you to store your food in a hospital refrigerator. Be sure to label it.
If you routinely take vitamin supplements, get your doctor’s permission to take them in the hospital. Even if you don’t take such supplements regularly, they might make sense for you in the hospital since your other nutritional intake may be deficient. Ask your doctor to arrange for your vitamins to be properly labeled, stored, and dispensed by the nursing staff.
Ask to see a hospital dietician if you have problems with food. Eat well, but be sure to follow orders about not eating before surgery.
Demand the Basic Comforts
 It is important to your recovery that you be as comfortable and happy as possible. If your roommate or the roommate’s visitors are too noisy, discuss it with your roommate. If that doesn’t work, or if something your roommate can’t control like incessant coughing is making it very difficult for you to relax or sleep, ask to have your room changed. If there is too much noise in the hall, ask what can be done about that. Another possible solution to noise problems is to use headphones while watching TV or listening to music.
It is important to your recovery that you be as comfortable and happy as possible. If your roommate or the roommate’s visitors are too noisy, discuss it with your roommate. If that doesn’t work, or if something your roommate can’t control like incessant coughing is making it very difficult for you to relax or sleep, ask to have your room changed. If there is too much noise in the hall, ask what can be done about that. Another possible solution to noise problems is to use headphones while watching TV or listening to music.
Negotiate about schedule. If the staff routinely wakes you up three times in the middle of the night, ask whether all those disturbances are needed. See if you can take the medication or have the readings taken right before bedtime or right after you wake up. If you are normally a late sleeper, see if your normal schedule can be accommodated. If you don’t want sleeping pills, ask not to be given them.
If you want someone to sleep-in with you, ask for that to be arranged. A comfortable chair should be provided, and many hospitals will provide cots.
Don’t Accept Treatment without Your Consent
You have a right—based on law and on medical ethics—to be treated only after giving your informed consent. Before surgery, you will be asked to sign a consent form. In the absence of consent, a surgeon’s cutting you open with a knife would be deemed negligence in some states, battery in others. Yet studies have found that substantial percentages of patients do not fully understand what their physicians have described about a procedure, and many would like more explanation.
If you don’t understand the risks, the benefits, the alternatives, and other important aspects of a procedure, ask for more information. Do this even if you have already signed a consent form. It is not too late to change your mind right up until the procedure begins. This applies not only to surgery, but also to radiology procedures, drug treatments, blood transfusions, and other procedures that may pose risks to you.
Consider Carefully Participation in Clinical Trials
 You may be offered a chance to participate in a clinical trial. A clinical trial is research in which the use of new drugs or medical devices is tested in humans. The purpose of such trials is to learn whether new treatments will benefit future patients.
You may be offered a chance to participate in a clinical trial. A clinical trial is research in which the use of new drugs or medical devices is tested in humans. The purpose of such trials is to learn whether new treatments will benefit future patients.
Although the new treatment being tested might be better than alternative treatments, it might be worse. Also, if you participate in a trial, you might be assigned to the “control” group that gets a standard treatment rather than the new treatment. (In cases of life-threatening disease, control groups virtually always get a treatment that has been judged to have some value, not just no treatment at all.) There is some evidence that patients who have participated in trials have survived longer than patients who chose to get treatment outside a trial. An explanation for such a difference might be that patients in a trial may receive closer medical attention and more follow-up visits than patients who are not in a trial.
A very valuable resource to help you make a decision about participation in a clinical trial is Should I Enter a Clinical Trial?, a guide prepared by the ECRI Institute, a nonprofit health services research organization. Drawing on the guide, we list below some of the types of information you will want to get to help you decide whether to participate in a clinical trial—
- A summary of results from previous trials that led to this trial.
- The purpose of the new research—what it is trying to achieve.
- How long the trial will last for you if you remain in it to the end.
- A detailed description of each test and treatment that will be given.
- The timing and the location of those tests and treatments and how they are scheduled for you.
- Identification of any procedures that are experimental.
- A description of any reasonably foreseeable risks or discomforts to you (for example, pain or minor and major side effects) from any test or treatment that will be given.
- A description of any possible benefits to you or to others.
- Information on whom to contact with questions about the trial and your rights.
- Information on whom to contact in the event of a research-related injury.
Have Your End-of-Life Wishes Prevail
 At some point, patients, their families, and friends may have to decide whether to extend life-sustaining treatment with measures such as resuscitation, endotracheal intubation, feeding tubes, and administration of IV fluids. If you want your end-of-life wishes honored, you will need to have discussions with your family or other representatives and your physician in advance. Good communication at the end of life can also help patients achieve closure and meaning in the final days of their lives.
At some point, patients, their families, and friends may have to decide whether to extend life-sustaining treatment with measures such as resuscitation, endotracheal intubation, feeding tubes, and administration of IV fluids. If you want your end-of-life wishes honored, you will need to have discussions with your family or other representatives and your physician in advance. Good communication at the end of life can also help patients achieve closure and meaning in the final days of their lives.
In 1990, the Federal Patient Self-Determination Act was passed by Congress to encourage competent adults to complete advance directives. The act requires hospitals, nursing homes, health maintenance organizations, and hospices that participate in Medicare and Medicaid to ask if patients have advance directives, to provide information about advance directives, and to incorporate advance directives into the medical record.
Advance directives are any expression by a patient intended to guide care, should the patient lose his or her medical decision-making capacity. Although both oral and written statements are valid, the added effort required to complete written statements gives them greater weight. In addition to their use when patients lose competence, advance directives also help patients consider the type of care they would want in the future, even if they retain decision-making capacity. Advance directives have legal validity in almost every state.
There are two principal forms of written advance directives: living wills and durable powers of attorney for healthcare. A living will is a document that allows you to indicate the interventions you would want if you were terminally ill, comatose with no reasonable hope of regaining consciousness, or in a persistent vegetative state with no reasonable hope of regaining significant cognitive function. A durable power of attorney for healthcare is a more comprehensive document that allows you to appoint a person as a proxy to make healthcare decisions for you should you lose decision-making capacity.
Unfortunately, the potential for advance directives to guide patient care is often not realized. Many patients don’t complete such directives, and often the directives are not available or adequately communicated at the time end-of-life decisions must be made. Even when a written advance directive document is prepared, it may not meet its objective. One study found that only 12 percent of patients with an advance directive had talked with a physician when completing the document and only 25 percent of physicians were aware of their patients’ advance directives. One study that surveyed elders in community settings found that 81 percent desired to discuss their preferences with their physicians if they were terminally ill, but only 11 percent had done so. In one survey of 200 patients, only 18 percent had filled out an advance directive and of these, 50 percent had secured the only copy in a safe deposit box.
Copies of advance directives often are not transferred from nursing homes to hospitals on admission. One study found that physicians documented advance directives or discussions with appointed proxies about treatment decisions in only 11 percent of admission notes. While 90 percent of Americans say they want to die at home, four out of five die in a hospital or other healthcare facility.
If you wish to have control over your own end-of-life decisions, you will need to discuss your preferences with your family and physician, complete the documentation, and make sure, on your own or through a representative, that the documentation is included in your medical record at hospitals or other care facilities you enter.
Leave with a Map
 Before it is time to leave the hospital, be sure you have a realistic plan for your care. Will you be able to care for yourself at home? Will you be able to get along with the help of an available family member? Will you need a visiting nurse or aide? Meals On Wheels? A nursing home? Make contact early, even before you enter a hospital if possible, with a hospital social worker and with other community social service agencies you are familiar with.
Before it is time to leave the hospital, be sure you have a realistic plan for your care. Will you be able to care for yourself at home? Will you be able to get along with the help of an available family member? Will you need a visiting nurse or aide? Meals On Wheels? A nursing home? Make contact early, even before you enter a hospital if possible, with a hospital social worker and with other community social service agencies you are familiar with.
You will also need to make sure that there is a plan for your medical care and management by a physician after you leave the hospital. Will you turn to your primary care doctor or to a specialist who treated you in the hospital? If a doctor other than the doctor who managed your care in the hospital will be responsible, you will need to take steps to ensure that the doctor who will be taking over has full information about you and your case right away.
That kind of information is supposed to be contained in a well-organized and thorough “discharge summary,” which is supposed to be communicated promptly to the doctor who will be caring for you. Unfortunately, it doesn’t always work that way.
Discharge summaries often are in a relatively unstructured, narrative format that invites inaccuracies. In addition, there can be significant delays transmitting discharge summaries to the doctors who need them.
In one study examining the effectiveness of inpatient follow-up care, nearly 10 percent of discharged patients experienced worsening of symptoms or functional capacity as a result of an inadequately managed discharge process. Another study demonstrated that patients may be less likely to be readmitted to the hospital if their primary care provider receives a discharge summary. Yet one study found that only 34 percent of patients had a discharge summary sent to their outpatient care provider.
Be active in planning the care you will receive after discharge. Before leaving the hospital, ask your doctor when a discharge summary will be prepared, to whom it will be sent, and how it will be sent. Ask that a copy be sent to you. Then keep track of whether you get one and check with your outpatient care provider to be sure that provider’s copy arrived.
Be Aware of Your Rights and Complain When Necessary
 If you feel you are not being treated with the proper respect or care, talk with the staff concerned. If that fails, talk with the nurse who works on the floor most regularly or with the head nurse on the floor. You can also check whether the hospital has a patient representative or ombudsman department. You can call a patient representative to talk about anything from cold food to rude staff. This person is charged with taking the problem to the responsible department and checking back with you to ensure that the problem is corrected.
If you feel you are not being treated with the proper respect or care, talk with the staff concerned. If that fails, talk with the nurse who works on the floor most regularly or with the head nurse on the floor. You can also check whether the hospital has a patient representative or ombudsman department. You can call a patient representative to talk about anything from cold food to rude staff. This person is charged with taking the problem to the responsible department and checking back with you to ensure that the problem is corrected.
To help you insist on the care you deserve, it is useful to know your rights as a patient. Every hospital should have a statement of patient rights. You might ask for a copy of this statement at the time of admission or before. It should cover such matters as the right to informed consent and participation in your medical care, the right to privacy during physical examination, and the right to refuse to participate in any hospital research experiments.
If you consider a complaint serious enough—you believe your health is in jeopardy or the quality of care is simply very bad—talk with your doctor about having you transferred to another unit of the hospital or another hospital, or just sending you home. The doctor should recognize that your tension or unhappiness is not making you feel any better, and should be willing to try something else.
Don’t Let Yourself Be Dumped
Because hospitals are paid by the case by Medicare and in a similar fashion by some other insurance plans, a hospital may come out better financially by discharging patients prematurely. Don’t let this happen to you. First, tell your doctor that you don’t feel well enough to go home. If he or she can’t or won’t stop the discharge process and if you are on Medicare, the hospital is required to give you a written description of an appeal procedure. During your appeal, which usually takes a day or two, you can stay in the hospital.

